All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the Lymphoma Coalition.
The Lymphoma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Lymphoma Hub cannot guarantee the accuracy of translated content. The Lymphoma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Lymphoma & CLL Hub is an independent medical education platform, sponsored by AbbVie, BeOne Medicines, Miltenyi Biomedicine, Nurix Therapeutics, Roche, Sobi, and Thermo Fisher Scientific and supported through educational grants from Bristol Myers Squibb, Eli Lilly, and Pfizer. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View lymphoma & CLL content recommended for you
ASH 2016 | Molecular Monitoring and Tailored Strategy with Pre-Emptive Rituximab Treatment for Molecular Relapse; Results from the Nordic Mantle Cell Lymphoma Studies (MCL2 and MCL3) with Median Follow-up of 8.5 Years
The 58th Annual Meeting & Exposition of the American Society of Hematology (ASH) took place in San Diego, CA, and on December 3rd, Arne Kolstad, MD, PhD, from Oslo University Hospital, Norway, presented results from the Nordic MCL Studies (MCL2 and MCL3) into pre-emptive rituximab treatment. Their goal was to assess the value of Minimal Residual Disease (MRD) monitoring to predict relapse in Mantle Cell Lymphoma (MCL) patients after Autologous Stem Cell Transplantation (ASCT) and in determining when to use pre-emotive rituximab.
Highlights:
- Treatment:
- 6 cycles of R-CHOP and R-Ara-C alternately, then high-dose ASCT
- Clinical + molecular evaluation 2-3 then 6 months after ASCT, then every 6 months
- MRD estimated by standard nested and quantitative RT-PCR
- Four weekly doses of 375mg/m2 rituximab was given to patients with clinical remission, but with molecular relapse
- Molecular relapse defined as either standard nested PCR changing to positive, or two consecutive samples showing >5 fold increase in RT-PCR MRD level

- Results:
- mFU = 8.5 years
- MRD-negative pts had longer Progression Free Survival (OS) and Overall Survival (OS) (P < 0.001)
- After 10 years 73% of the 86 pts in molecular remission had clinical remission
- 58 pts received rituximab after MRD relapse, 87% were converted back into remission
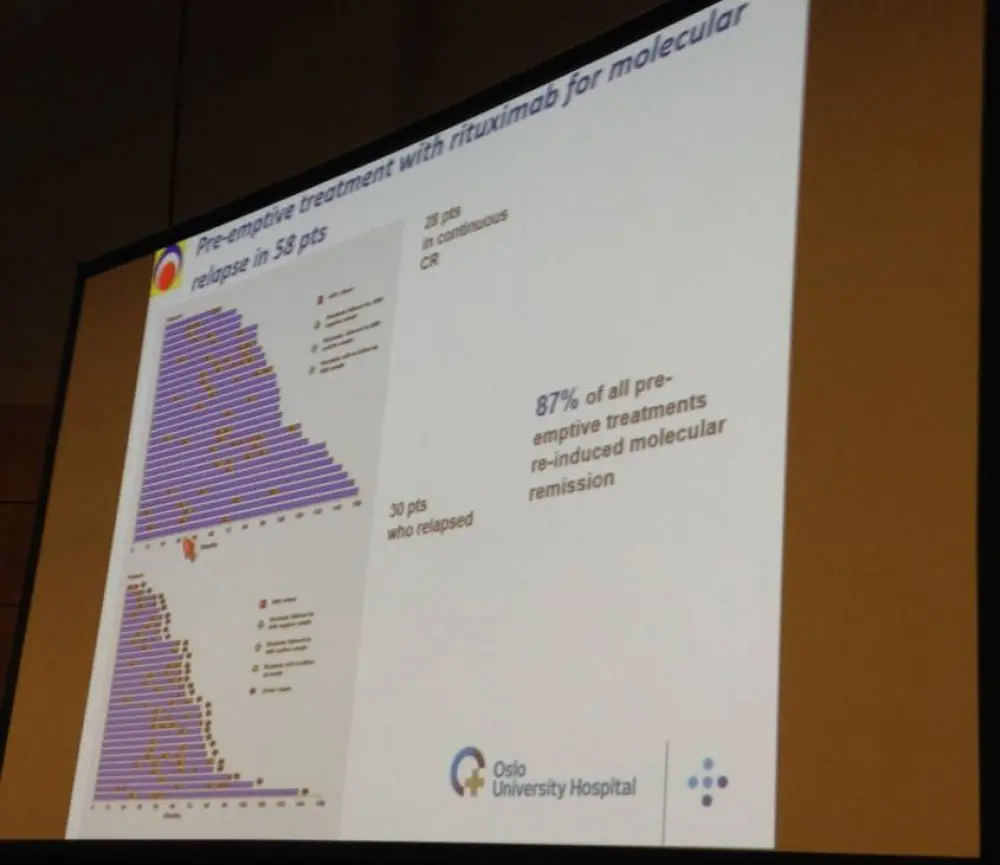
- Time from molecular to clinical relapse = 55 months (median)
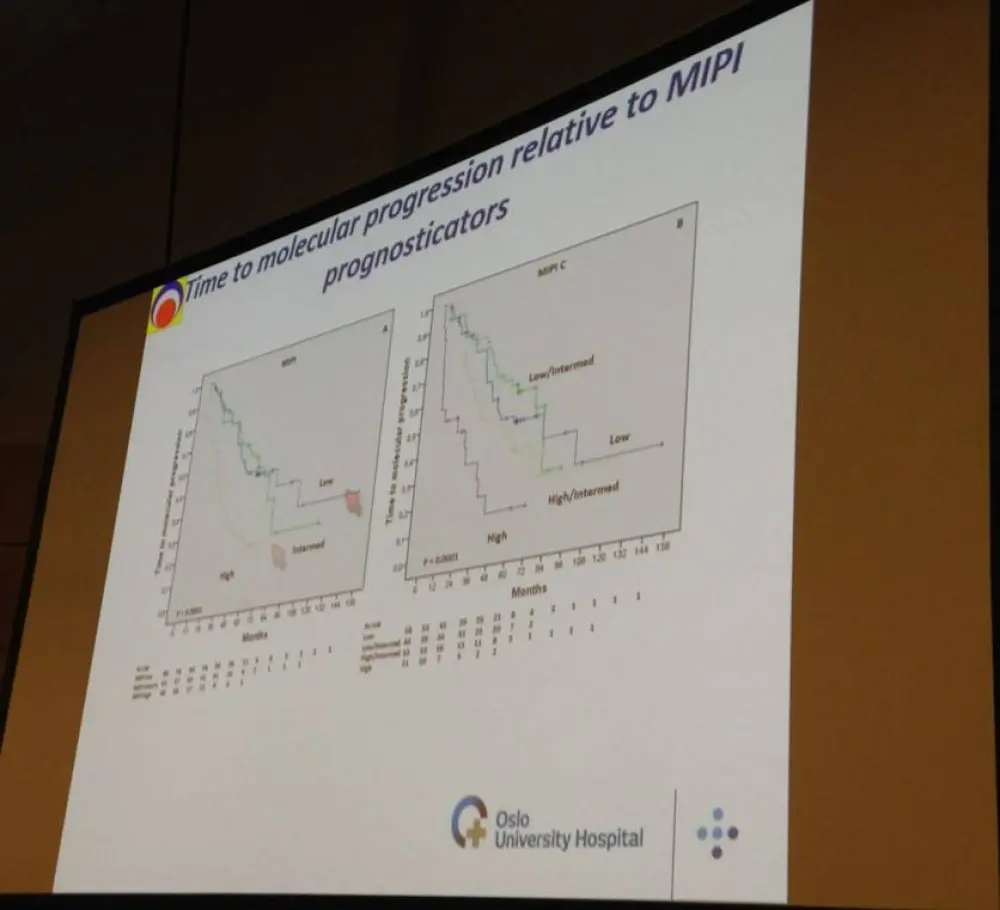
- MIPI high-risk categorization at diagnosis (P = 0.0001) and MRD discovery before ASCT (P = 0.0005) were both significant predictors of molecular relapse
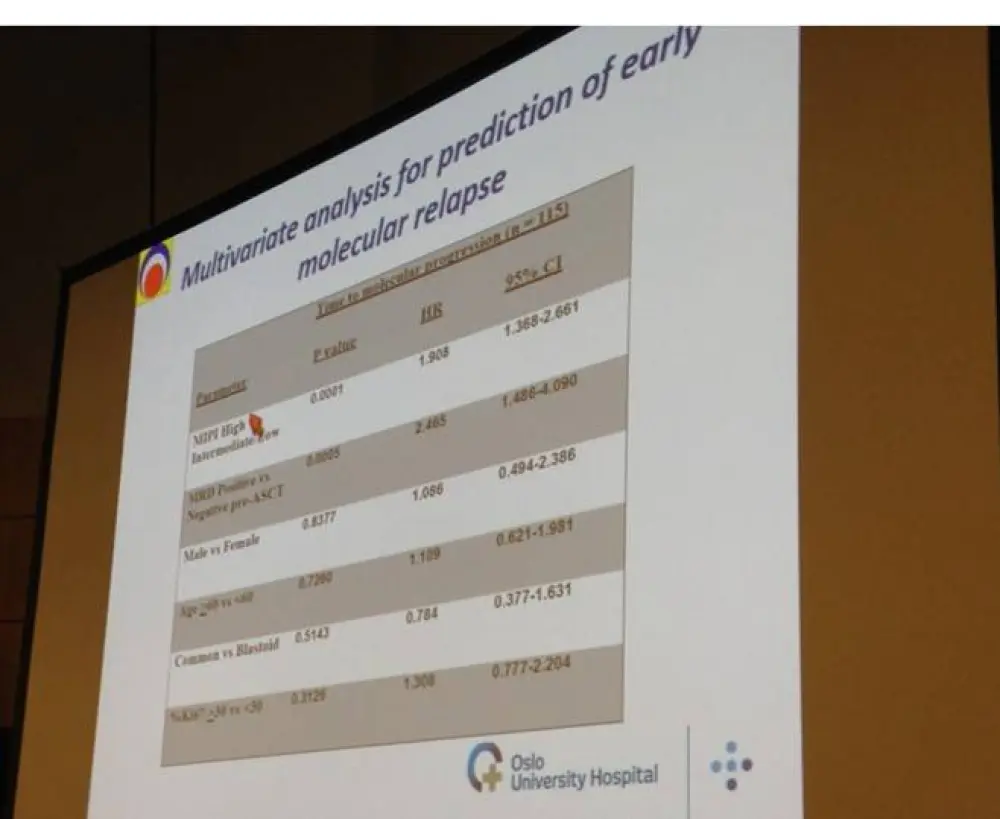

The authors of the study concluded that MCL should be considered a ‘chronic incurable lymphoma’. Furthermore, they stated that their data showed that MRD is a valuable predictor of survival and clinical relapse, and that pre-emptive rituximab delayed the clinical relapse identified by MRD.

Abstract:
Background: Minimal residual disease monitoring has been shown to be of relevance in mantle cell lymphoma (MCL) to evaluate quality of remission and predict clinical relapse. The main objectives of the present study were to determine the value of minimal residual disease (MRD) monitoring to guide pre-emptive treatment with rituximab, and to predict clinical relapse in MCL following autologous stem cell transplantation (ASCT) in two prospective trials (MCL2 and MCL3) with long-term follow-up conducted by the Nordic Lymphoma Group.
Methods: Patients treated in the two studies received a total of 6 alternating cycles with R-CHOP and R-Ara-C followed by a peripheral blood stem cell harvest and high-dose therapy with ASCT. Additionally, responding patients not in CR before ASCT in the MCL3 trial received yttium-90 ibritumomab tiuxetan (0.4 mCi/kg) as intensification one week prior to the standard conditioning with BEAM/C. Staging included physical examination, blood tests, computed tomography (CT) scans and bone marrow (BM) aspiration and biopsy. Clinical and molecular response evaluation was repeated 2-3 months and 6 months after transplant, and then every 6 months until relapse or 5 years follow-up. A combined standard nested and quantitative real-time PCR assay was used to estimate MRD involvement in consecutive post-transplant BM/PB samples. Molecular relapse after ASCT was defined as; 1. Conversion from standard nested PCR negative to standard nested PCR positive, or 2. For patients who were MRD positive post-ASCT, a significant (>5 fold) increase of the real time quantitative PCR detectable MRD level in two consecutive BM samples. Patients in clinical remission who developed a molecular relapse in both studies received 4 weekly doses of rituximab (375 mg/m2). This treatment could be repeated in case of recurrent molecular relapses.
Results: An MRD marker for Bcl-1 or IgH rearrangement was obtained for 94 out of 160 patients (59%) recruited in the Nordic MCL2 trial, and for 121 out of 160 (76%) in the consecutive MCL3 trial. 183 patients, who had completed induction therapy and autologous stem cell transplantation (ASCT) in the two studies and where a PCR marker in blood or bone marrow was obtained, were included in the current analysis. Median follow-up from inclusion was 8.5 years among survivors. Patients who were MRD negative post-ASCT had significantly longer relapse-free survival (RFS) and overall survival (OS) compared to those who were MRD positive (P<0.001). Eighty-six patients remained in continuous molecular remission. Of those, 73% also remained in clinical remission after 10 years. For all patients, median time from ASCT to molecular relapse was 55 months and with no signs of a plateau on the curve (Figure 1). Fifty-eight patients with MRD relapse received pre-emptive treatment with 4 weekly doses of rituximab (375 mg/m2) on one or more occasions. Conversion back to MRD negative state was achieved in the majority (82%) of cases after rituximab treatment. Median time from molecular relapse to clinical relapse in patients who received pre-emptive rituximab was 55 months (Figure 2). In a multivariate analysis, significant predictors for molecular relapse were MIPI high risk category at diagnosis (HR 1.91, 95% CI 1.37-2.66, P=0,0001) and detection of MRD prior to ASCT (HR 2.47, 95% CI 1.49-4.09, P=0.0005). Late MRD relapses continued to occur 5-10 years after ASCT even in lower risk groups.
Conclusion: We observed a continuous pattern of MRD relapses that did not subside even after 5-10 years and included all risk groups. Hence, it is fair to consider MCL as a chronic incurable lymphoma entity and novel approaches will be necessary to change the natural course of this disease. Detection of MRD was shown to be a predictor for clinical relapse and inferior survival. Additionally, the data strongly suggests that pre-emptive rituximab treatment delayed clinical relapse in MCL. We recommend MRD monitoring post-ASCT in MCL as a useful approach to select the MRD positive patients for novel strategies in future trials and as an alternative to maintenance therapy for all patients. The MCL2 and MCL3 trials were registered at www.isrctn.com as ISRCTN 87866680 and at www.clinicaltrials.gov as NTC 00514475, respectively.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content

