All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the Lymphoma Coalition.
The Lymphoma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Lymphoma Hub cannot guarantee the accuracy of translated content. The Lymphoma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Lymphoma & CLL Hub is an independent medical education platform, sponsored by AbbVie, BeOne Medicines, Miltenyi Biomedicine, Nurix Therapeutics, Roche, Sobi, and Thermo Fisher Scientific and supported through educational grants from Bristol Myers Squibb, Eli Lilly, and Pfizer. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View lymphoma & CLL content recommended for you
ASH 2016 | Durable Remissions with the VcR-CVAD Regimen for Mantle Cell Lymphoma (MCL), Regardless of Age: Long-Term Follow-up of a Wisconsin Oncology Network (WON) Study
The 58th Annual Meeting & Exposition of the American Society of Hematology’s (ASH) took place in San Diego, CA, and on December 3rd, Julie Chang, MD, of the University of Wisconsin School of Medicine and Public Health, presented long-term follow-up data from a study based on the addition of bortezomib, with maintenance rituximab, to modified hyper-CVAD chemotherapy in patients with untreated Mantle Cell Lymphoma (MCL). This update session included data after 5 years of maintenance rituximab, building on previous data and publications.
Highlights:
- VcR-CVAD = Induction chemotherapy with Bortezomib, cyclophosphamide, rituximab, vincristine, doxorubicin, and dexamethasone, with maintenance rituximab beyond 2 years

- At 3 years ORR = 90%, PFS = 63% and OS = 86%
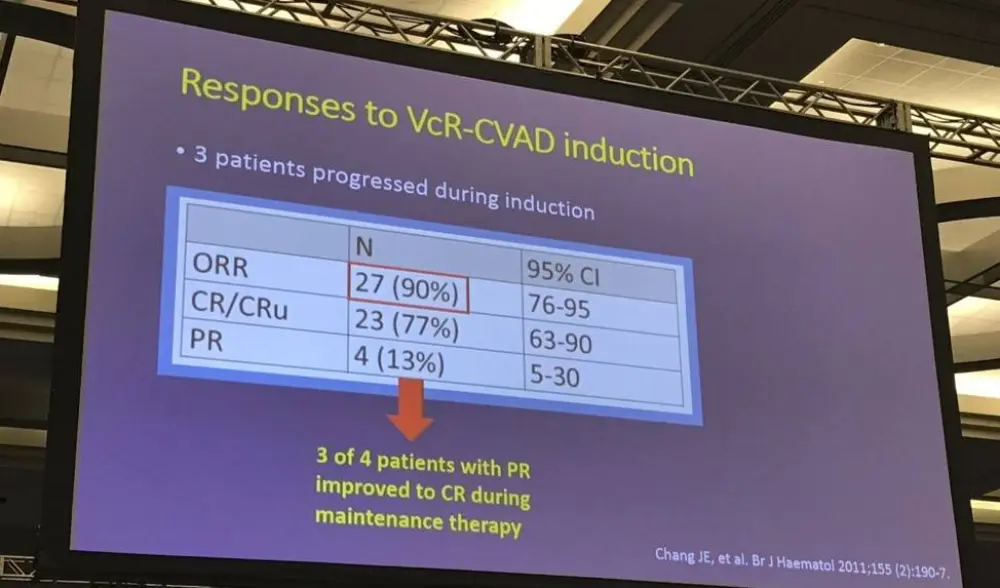
- Of 30 pts enrolled, 20 were alive at median follow-up of 7.8 years, 15 in ongoing remission
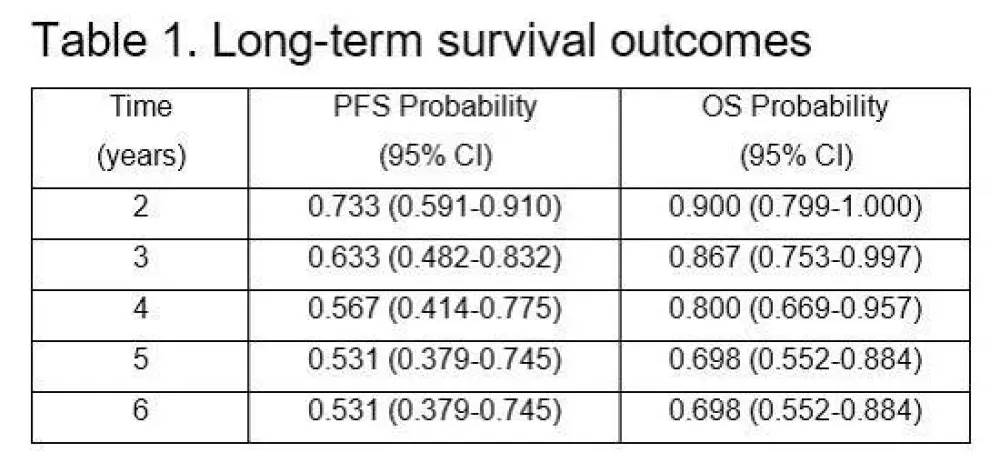
- Estimated 6 year PFS = 53.1% and OS = 69.8% (95% CI)
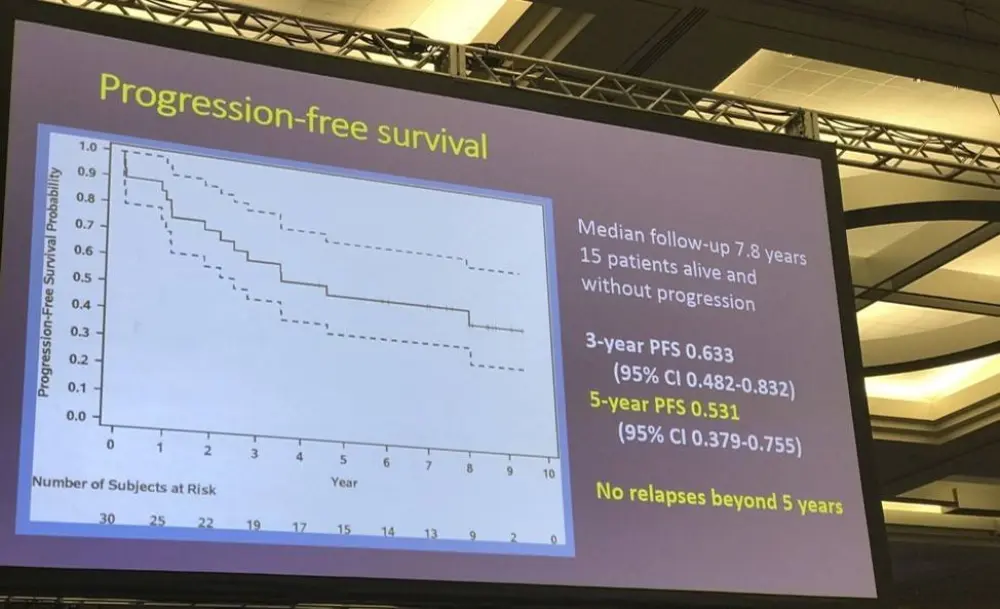
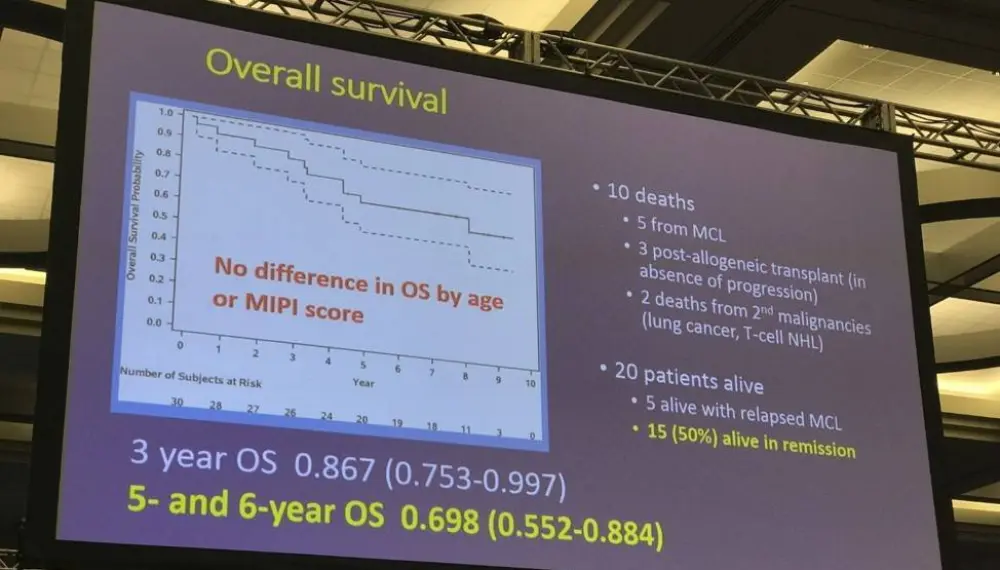
- No significant differences in OS or PFS when those under and over 60 were compared
- No late toxicities reported during the long term follow-up
In conclusion, Julie Chang stated that VcR-CVAD with 5- years maintenance rituximab was able to demonstrate durable remission, comparable to intensive chemotherapy and ASCT, and is tolerable in older and less fit patients.

Abstract
Introduction: There remains no clear standard first-line therapy for MCL. VcR-CVAD is a novel, intermediate-intensity chemoimmunotherapy regimen which incorporates bortezomib into modified hyper-CVAD chemotherapy. We hypothesized that the addition of bortezomib would improve the complete response (CR) rate, and maintenance rituximab (MR) would improve the remission duration. The results of this study were previously reported (Chang JE, et al. Br J Haematol 2011), with an observed overall response rate (ORR) of 90% (CR/unconfirmed CR in 77%), and 3-year progression-free survival (PFS) and overall survival (OS) of 63% and 86%, respectively. Long-term follow-up (LTFU) is reported from this multicenter trial.
Methods: The study enrolled patients ≥18 years of age with histologically confirmed MCL. Patients were previously untreated, with the exception of 1 cycle of CHOP/CHOP-like chemotherapy. Patients received VcR-CVAD induction chemotherapy every 21 days for 6 cycles: rituximab (R) 375 mg/m2 intravenously (IV) on day 1; bortezomib/Velcade® (Vc) 1.3 mg/m2 IV, days 1 & 4; cyclophosphamide 300 mg/m2 IV every 12 hours, days 1-3 (total of 6 doses); doxorubicin 50 mg/m2 IV continuous infusion days 1-2 (total dose over 48 hours equal to 50 mg/m2); vincristine 1 mg IV day 3; and dexamethasone 40 mg orally days 1-4. Patients received G-CSF support beginning day 5-6 of each induction cycle, and all appropriate supportive care measures were permitted throughout treatment including tumor lysis prophylaxis, transfusion support and antibiotics. Patients achieving at least a partial response to induction therapy received R consolidation (R 375 mg/m2 IV X 4 weekly doses) and MR (R 375 mg/m2 IV every 12 weeks for a total of 5 years; total of 20 doses). Restaging CT scans were performed after cycles 2, 4, and 6 of induction, 12 weeks after consolidation, every 6 months during maintenance, and yearly during LTFU. The primary endpoint was ORR and CR to induction chemotherapy; secondary endpoints were PFS and OS.
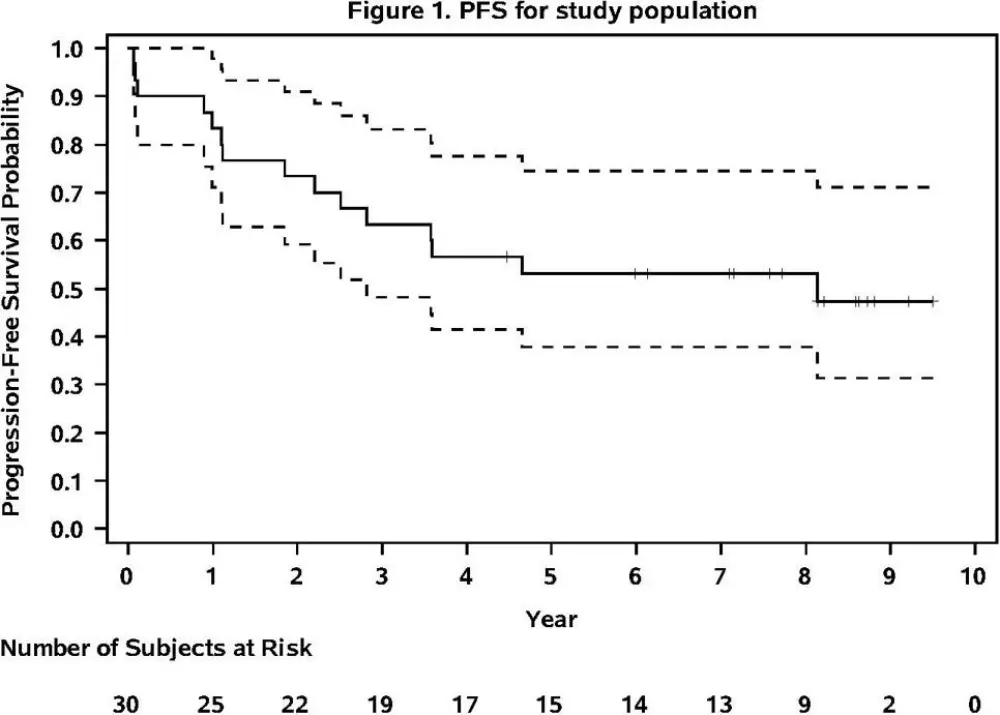
Results: Thirty patients were enrolled from 7/2005-5/2008. Median age was 61 years (range 48-74), 80% male, all patients had advanced stage disease, and 60% had MIPI score of medium- or high-risk disease. Six patients had blastic morphology. Long-term results are reported after a median follow-up of 7.8 years in surviving patients. Twenty patients are alive, and 15 (50%) are alive in ongoing remission (Figure 1). Estimates of 6-year PFS and OS are 53.1% and 69.8%, respectively (Table 1). The observed PFS and OS differences between patients <age 60 and those ≥age 60 were not statistically significant. The observed PFS and OS differences by MIPI score were not statistically significant, although there was a trend towards worse PFS and OS for high-risk MIPI patients. Five patients have died from confirmed progression of MCL. Two deaths occurred from complications post-allogeneic transplant, and 3 deaths occurred from unrelated causes with MCL in remission. No MCL relapses have been observed beyond 5 years. No late toxicities from VcR-CVAD or from MR have emerged during the LTFU.
Conclusions: VcR-CVAD is a moderate intensity chemotherapy regimen that is tolerable for many older and less fit adult patients as first-line therapy of MCL. LTFU of patients receiving VcR-CVAD induction followed by 5 years of MR demonstrates high rates of durable remission that are comparable with more intensive chemotherapy and consolidative autologous stem cell transplant (ASCT). The highly promising activity of the VcR-CVAD regimen was recapitulated in ECOG-ACRIN protocol E1405 (Chang et al, Blood 2014). A randomized phase 3 trial has recently confirmed the beneficial effects of bortezomib incorporation into standard immunochemotherapy (Robak et al, NEJM 2015). VcR-CVAD remains an effective therapy choice for initial treatment of MCL, both in younger and older MCL populations.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content
Your opinion matters
In your experience, what is the average vein-to-vein time when treating patients with DLBCL with a reimbursed CAR T-cell therapy (from apheresis to infusion)?

