All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the Lymphoma Coalition.
The Lymphoma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Lymphoma Hub cannot guarantee the accuracy of translated content. The Lymphoma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Lymphoma & CLL Hub is an independent medical education platform, sponsored by AbbVie, BeOne Medicines, Miltenyi Biomedicine, Nurix Therapeutics, Roche, Sobi, and Thermo Fisher Scientific and supported through educational grants from Bristol Myers Squibb, Eli Lilly, and Pfizer. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View lymphoma & CLL content recommended for you
Responses to the SARS-CoV-2 booster vaccination in patients with lymphoid malignancies
Do you know... For patients with lymphoid malignancies who failed to respond to two previous COVID-19 vaccine doses, which of these factors is associated with increased likelihood of seropositivity following a third COVID-19 vaccine dose?
The immunosuppressive effect of active treatment and disease in patients with lymphoid malignancies has proven to impair immune response to the first two doses of SARS-CoV-2 vaccination.1,2 It is of value to determine whether a booster vaccination can improve antibody responses and whether certain subgroups of patients may benefit more than others from a third vaccine dose. Additionally, T-cell-mediated responses, even in the absence of seroconversion, may also infer an advantage to receiving a booster vaccine.2 We have previously summarized an evaluation of these responses following a second vaccine dose.
Here, we provide a summary of two papers investigating humoral and T-cell-mediated responses in patients with lymphoid malignancies receiving a third BNT162b2 vaccine dose. 1,2
Seroconversion in patients with B-cell non-Hodgkin lymphoma1
A retrospective study (NCT04746092) published by Avivi et al. in the British Journal of Hematology observed the seroconversion rate of anti-SARS-CoV-2 spike antibodies in 44 patients with B-cell non-Hodgkin lymphoma (B-NHL) receiving a BNT162b2 booster vaccine who failed to respond to two previous doses of SARS-CoV-2 vaccination.
Baseline characteristics are summarized in Table 1.
Table 1. Baseline patient characteristics*
|
B-NHL, B-cell non-Hodgkin lymphoma; CR, complete remission; DLBCL, diffuse large B-cell lymphoma; IQR, interquartile range; PD, progressive disease; PR, partial response; SD, stable disease. |
|
|
Characteristic |
N = 44 |
|---|---|
|
Median age, years (IQR) |
66 (55–73) |
|
Subtype, % |
|
|
DLBCL |
36.4 |
|
Other B-NHL† |
63.6 |
|
Disease status |
|
|
CR |
84 |
|
PR |
4.5 |
|
SD |
7 |
|
PD |
4.5 |
|
Treated with anti-CD20 mAbs, % |
95.5 |
|
Current maintenance therapy, % |
46 |
|
Median absolute lymphocyte count, × 103/µL (IQR) |
1.2 (0.7–1.5) |
|
≤6 months from previous anti-CD20 mAb, % |
45.2 |
Results
- Following the booster vaccination, 13 patients achieved a serological response (29.54%).
- Receiving an anti-CD20 mAb treatment ≥6 months prior to the vaccine dose and DLBCL subtype were both associated with greater seropositivity (Figure 1).
- Of the 28 patients with other B-NHLs, 13 were receiving active maintenance treatment at the time of their third dose, and none of these patients achieved a seropositive result.
- There was a better response to the booster vaccine for patients not receiving maintenance treatment, with five of 15 patients achieving seropositivity (p = 0.031).
- In a multivariate analysis, lymphoma subtype (DLBCL vs other B-NHL; hazard ratio [HR], 5.55; 95% confidence interval [CI], 1.71–4.58; p = 0.032) and time from last exposure to anti CD20 mAb therapy (>6 months vs ≤6 months; HR, 6.51; 95% CI, 1.84–4.19; p = 0.04), maintained their significant association.
Figure 1. Seropositivity rates according to time from previous anti-CD20 treatment and type of B-NHL*
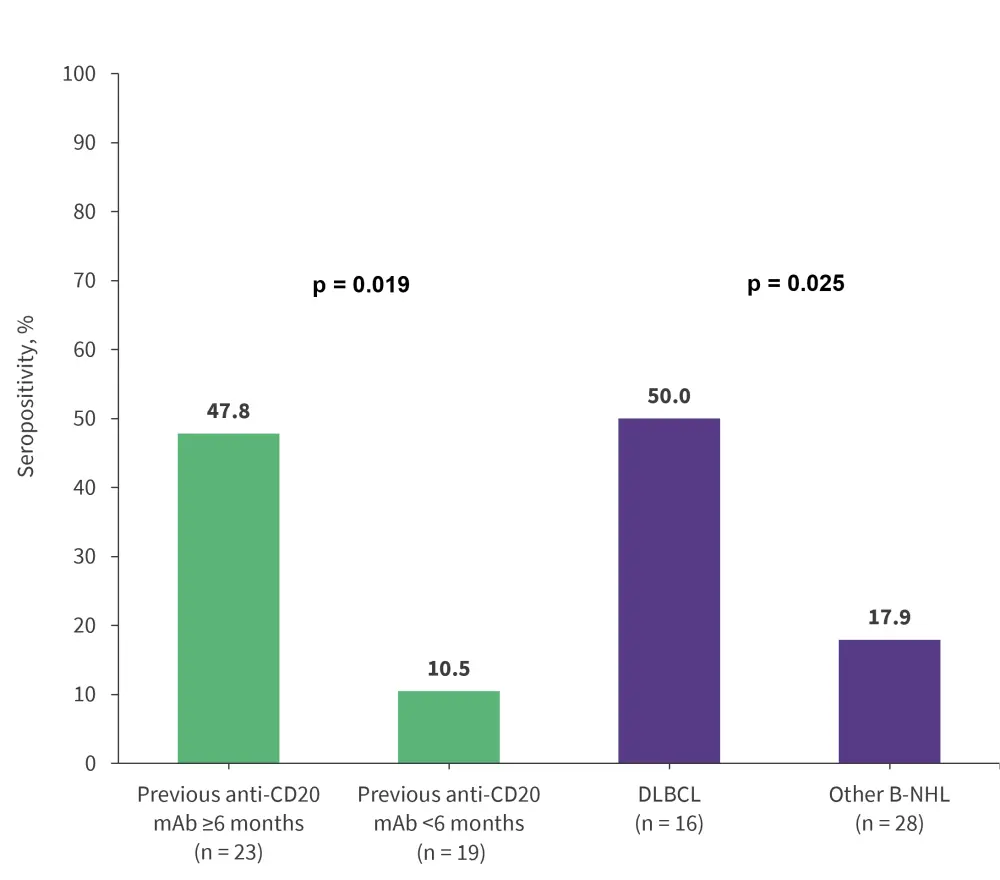
B-NHL, B-cell non-Hodgkin lymphoma; DLBCL, diffuse large B-cell lymphoma; mAB, monoclonal antibody.
*Adapted from Avivi, et al.1
- Notably, in a median follow-up period of 56 days, no cases of COVID-19 infection were reported.
Safety
- The booster vaccine was well tolerated, with a total of 28 patients (68.3%) experiencing a vaccine-related adverse event (AE), which were all Grade 1–2 and transient.
- The most common AE was pain at the injection site (n = 26; 63.4%).
- The most common systemic AEs were fatigue (n = 9; 22%) and headache (n = 6; 14.6%).
- Importantly, no difference in the prevalence and severity of AEs was observed between the first two doses and the booster vaccine.
In summary, this study demonstrated a high prevalence of seroconversion following a third SARS-CoV-2 vaccine dose in patients with B-NHL who failed to respond the first two doses, particularly for patients harboring aggressive B-NHL and those whose anti-CD20 mAb treatment ceased ≥6 months before vaccination.
Study limitations included the small cohort number, alonger period of time from the previous vaccine booster compared to similar studies, and the absence of T-cell-mediated immune response evaluation.
Cellular and humoral responses following a booster vaccine2
An observational study on the effect of a third BNT162b2 vaccine dose on SARS-CoV-2 anti-spike (anti-S) antibody (Ab) production, neutralizing capacity, and T-cell-mediated responses was recently published by Re et al. in Nature Communications. This study included patients with chronic lymphocytic leukemia (CLL), B-NHL, and multiple myeloma (MM) with poor or no response to their first two vaccine doses.2
Results
Patient characteristics are summarized in Table 2.
Table 2. Patient characteristics*
|
Abs, antibodies; anti-S, anti-spike; CLL, chronic lymphocytic leukemia; mAb, monoclonal antibody; MM, multiple myeloma; NHL, non-Hodgkin Lymphoma. |
|
|
Characteristic |
N = 43 |
|---|---|
|
No anti-S Abs before booster dose, % |
41.8 |
|
Median Ab titer in patients with Abs before booster dose, U/ml (range) |
87.1 (1.2–693) |
|
Median age, years (range) |
77 (37–92) |
|
Type of lymphoid malignancy, n |
|
|
MM |
16 |
|
NHL |
14 |
|
CLL |
13 |
Humoral response
- All 18 patients who tested negative for anti-S Abs prior to the booster vaccine dose remained negative following their third dose.
- A total of 14 of these patients had received a prior mAb treatment, and nine of those patients had received treatment within 12 months prior to the booster vaccine.
- All the 25 patients with a positive anti-S result prior to the booster vaccine remained positive following the vaccine dose.
- A total of 23 (92%) had a significant increase in the median antibody titer after their third dose (87.1 U/mL [range, 1.2–693] to 3,386 U/mL [range, 6.6–20312]; p < 0.001).
- When stratifying according to disease, patients with MM had the greatest change in median antibody titers from dose two to dose three (100 U/mL [range, 0–690] and 2,700 U/mL [range, 0–20,312]; p < 0.0001).
- Of the 25 patients with anti-S Abs before their third vaccine dose, 11 had neutralizing antibodies, meaning an ability to block entry of SARS-CoV-2 into cells via ACE-2 receptor binding.
- The number of patients with neutralizing antibodies increased to 21 after a third dose.
- The median neutralizing capacity of these patients increased from 18.5% to 96.3%.
Cellular response
- T-cell-mediated responses were evaluated in all patients irrespective of anti-S Ab positivity.
- Prior to the third dose, five out of 13 patients with no anti-S Abs had a positive result for T-cell response, and the investigators observed an increase to eight patients after the booster vaccine.
- Of the nine patients with a positive anti-S response prior to the booster vaccine, six had had a T-cell response, which remained the same following the booster.
- Five patients overall were double negative for humoral and T-cell-mediated responses.
- Of these five patients, three had a diagnosis of CLL, two had B-NHL, and four were undergoing active treatment.
- The median IFN-γ levels were increased overall following the booster vaccine.
- Unlike humoral responses, IFN-γ secretion was not affected by the time interval between previous anti-CD20 mAb treatment and the vaccine dose.
- Active treatment in patients with NHL and CLL impaired T-cell responses with a median IFN-γ secretion following exposure of 0.0 IU/mL (range, 0.0–0.5) vs 0.9 IU/mL (range, 0.1–4.0) in patients not on active treatment (p = 0.049).
Responses in patients with lymphoid malignancies vs healthy donors
- The investigators next compared immune response of 22 patients with CLL and NHL receiving the vaccine booster with healthy donors who had received two doses.
- There was comparable response in patients with CLL and NHL after their third dose and healthy donors who had received two doses.
- This included no significant difference in anti-S Ab titers, neutralization, and IFN-γ secretion following exposure to two SARS-CoV-2 antigens.
Safety
- The vaccine booster was well tolerated, with no additional adverse events reported in the 3–5-week follow-up, and only transient Grade 1–2 AEs reported.
In summary, a third dose of the BNT162b2 vaccine was beneficial for patients who had previous anti-S Ab responses, who had improved median Ab titer. This effect was greater in patients with MM compared to those with CLL or NHL. A considerable number of these patients without a humoral response were positive for T-cell-mediated responses after the booster vaccine.
Conclusion
Overall, these two studies support the use of a third vaccine dose in patients with lymphoid malignancies. Some selective factors, including shorter time from previous anti-CD20 treatment and active maintenance therapy in patients with B-NHL impaired seroconversion. However, T-cell-mediated immune activity may still provide important protection and was improved with a booster vaccine.
Your opinion matters
In your current clinical practice, how likely would you be to recommend a booster COVID-19 vaccine for your patients with lymphoid malignancies who have failed to respond to two previous COVID-19 vaccine doses?
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content
Your opinion matters
In your experience, what is the average vein-to-vein time when treating patients with DLBCL with a reimbursed CAR T-cell therapy (from apheresis to infusion)?

