All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the Lymphoma Coalition.
The Lymphoma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Lymphoma Hub cannot guarantee the accuracy of translated content. The Lymphoma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Lymphoma & CLL Hub is an independent medical education platform, sponsored by AbbVie, BeOne Medicines, Miltenyi Biomedicine, Nurix Therapeutics, Roche, Sobi and Thermo Fisher Scientific and supported through independent educational grants from Bristol Myers Squibb, Incyte, Lilly, and Pfizer. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View lymphoma & CLL content recommended for you
Venetoclax for del(17p) chronic lymphocytic leukemia: Long-term follow-up data from the M13-982 trial
The phase II M13-982 trial (NCT01889186) assessed venetoclax monotherapy in patients aged ≥18 years with relapsed/refractory (R/R) or previously untreated chronic lymphocytic leukemia (CLL) with a 17p deletion (del[17p]).1 The study design and primary results have previously been reported by the Lymphoma Hub. Briefly, venetoclax was associated with an overall response rate (ORR) of 77% and was well tolerated.1 Here, we summarize the 6-year follow-up and subgroup analyses from the M13-982 trial, published by Stilgenbauer, et al.1 in Blood Advances.
Study design and patient population
- This was an open-label, multicenter, phase II trial of patients with R/R CLL.
- Following dose ramp-up, patients received 400 mg venetoclax once daily continuously.
- Post hoc subgroup analyses of outcomes were conducted in genetically defined subgroups.
- To assess continuous single-agent venetoclax for ≥2 years vs time-limited venetoclax plus rituximab in patients with R/R CLL with del(17p)/TP53 mutations, outcomes were compared with the phase III MURANO trial (NCT02005471).
- Study endpoints included complete remission (CR) rate, partial remission (PR) rate, duration of response (DOR), progression-free survival (PFS), overall survival (OS), and safety.
Key findings
- Overall, 158 patients with R/R CLL (n = 153) and previously untreated CLL (n = 5) were included.
Efficacy
- At a median follow-up of 70 months, the ORR was 77% (Table 1).
Table 1. Response rates in the M13-982 trial*
|
*Data from Stilgenbauer et al.1 |
|
|
Response rate, % |
Venetoclax monotherapy |
|---|---|
|
Overall response rate |
77 |
|
Complete remission |
21 |
|
Complete remission with incomplete hematological recovery |
3 |
|
Partial remission |
49 |
|
Nodular partial remission |
4 |
|
Stable disease |
19 |
|
Progressive disease |
2 |
|
Not evaluable |
2 |
- Among responders, the median duration of response was 39.3 months (95% confidence interval [CI]: 31.1–50.5).
- Median progression-free survival (PFS) and overall survival (OS) are shown in Figure 1.
- The actuarial 5-year PFS and OS rates were 24% and 52%, respectively.
Figure 1. Long-term survival outcomes in M13-982 trial*
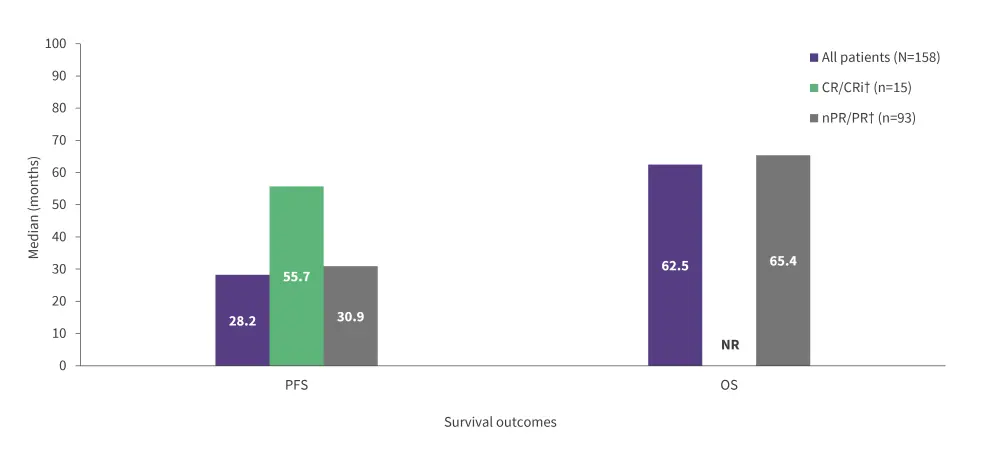
CR, complete remission; CRi, CR with incomplete hematological recovery; nPR, nodular partial remission; NR, not reached; OS, overall survival; PFS, progression-free survival; PR, partial remission.
*Data from Stilgenbauer et al.1
†Response at Week 36 (±4 weeks)
Safety
- No new safety signals were observed in this analysis.
- 98% and 89% of patients experienced any-grade and Grade ≥3 treatment-emergent adverse events, respectively.
- The most common Grade ≥3 treatment-emergent adverse events were neutropenia (42%), infections (33%), anemia (16%), and thrombocytopenia (16%).
- Adverse events resulting in a dose reduction occurred in 18% of patients.
Post hoc genetic subgroup analysis
- In the univariate analysis, the median PFS was higher in patients with unmutated SF3B1 vs mutated SF3B1 (30.2 vs 16.4 months; p = 0.0071).
- Multivariable analysis showed that ≥2 prior therapies, unmutated IGHV, nodal size ≥5 cm, SF3B1 mutated, and ≥2 TP53 mutations did not significantly impact ORR and PFS.
Post hoc comparative analysis of M13-982 and MURANO
- Median PFS from treatment initiation was 27.6 months (95% CI: 22.8–37.1) in the M13-982 cohort, while the median PFS from randomization was 37.4 months (95% CI: 29.4–52.3) in the MURANO cohort.
- The estimated 60-month OS rates were 50.6% and 70.2% in the M13-982 and MURANO cohorts, respectively.
- Median PFS by MRD status in patients who received ≥2 years of venetoclax in both trials is shown in Figure 2.
Figure 2. Median PFS from month 24 by MRD status in the M13-982 and MURANO trials*
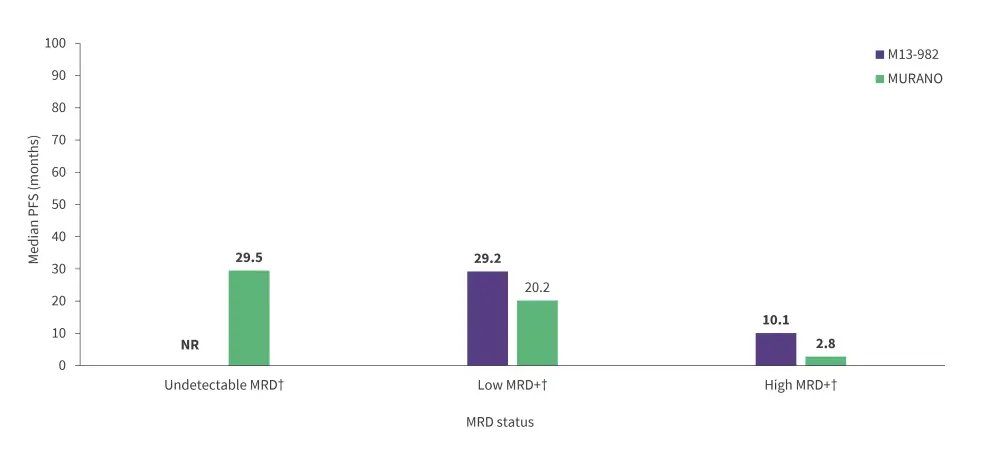
MRD, measurable residual disease; NR, not reached; PFS, progression-free survival.
*Data from Stilgenbauer et al.1
†MRD status was classified as undetectable (<10−4), low MRD positive (MRD+, 10−4 to 10–2), and high MRD+ (>10−2).
| Key learnings |
|
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content
Your opinion matters
What is the primary reason you use bridging therapy in patients with DLBCL awaiting CAR T-cell therapy?




